Key Takeaways
- Body acne is common in teenagers and adults, and it often behaves differently than facial breakouts.
- Breakouts on the back, chest, shoulders, and buttocks usually involve a mix of hormones, sweat, friction, and inflammation.
- Texture changes and post-acne marks can linger because the skin on the body is thicker and harder to treat consistently.
- Home care can work for mild cases, but recurring or painful flares often respond best to a structured plan.
- Professional care can reduce active breakouts, improve skin comfort, and lower the risk of scarring.
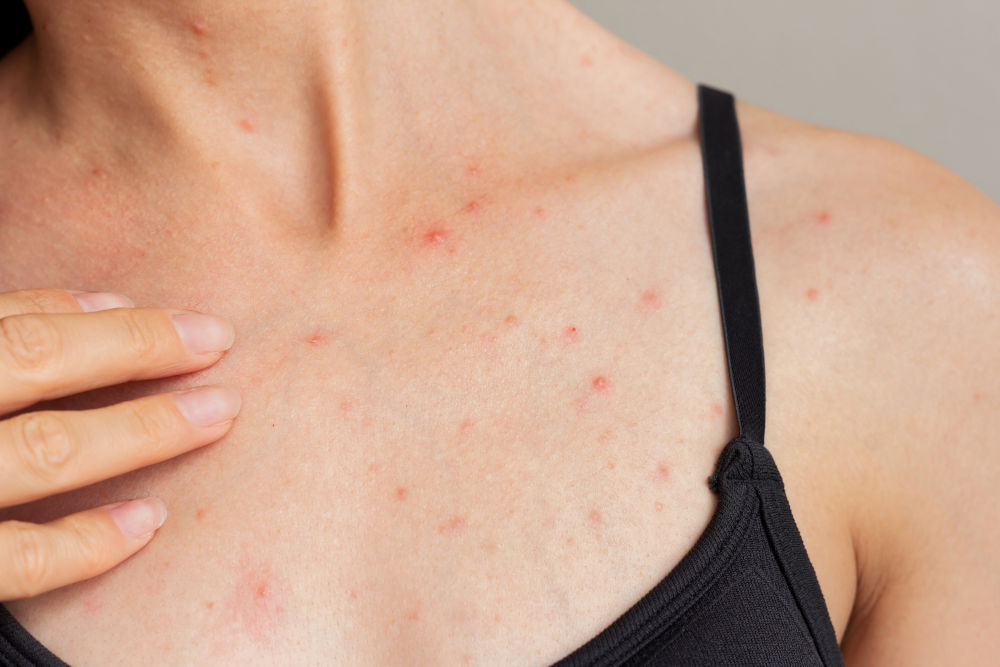
What Is Body Acne?
This condition is inflammation within hair follicles and pores on areas other than the face. The most typical sites are the back (“bacne”), chest, shoulders, upper arms, and buttocks. In clinic, Dinara often frames it in practical terms: it is not “dirty skin” or poor hygiene — it is a combination of follicle blockage, bacteria, and an inflammatory response that becomes self-sustaining if triggers keep repeating.
Compared with facial acne, the skin on the torso is thicker and follicles can sit deeper. That matters because clogged pores may form further below the surface and take longer to settle. It also means that acne on the body can leave darker marks or uneven texture more easily, especially when lesions are picked, scrubbed, or repeatedly irritated by clothing.
Common Causes of Body Acne
Hormonal Imbalances
Hormones influence oil production and skin inflammation. Androgens can increase sebum output and make pores more likely to clog. This is why flare-ups often track with adolescence, cycle changes, postpartum shifts, perimenopause, or stressful periods where sleep and recovery are disrupted.
Dinara’s clinical note here is simple: hormone-driven breakouts rarely respond to “stronger cleansers.” When hormones are the dominant driver, the plan needs to focus on reducing inflammation and preventing repeated clogging, not stripping the skin.
This pattern is often described as hormonal acne, and it can show up on the jawline, chest, or back depending on the person.
Stress and Cortisol
Stress is not always the root cause, but it can worsen existing breakouts. Elevated cortisol can increase inflammation and indirectly affect oil production and barrier function. Patients often notice that breakouts heal more slowly during high-stress weeks, even if their routine hasn’t changed.
If you are experiencing recurrent flares, it’s usually less helpful to ask “Did stress cause this?” and more helpful to ask: “Is stress keeping my skin inflamed and reactive?”
Friction and Tight Clothing
Friction-related breakouts are extremely common and under-recognised. Repeated rubbing and heat create an occlusive environment that traps sweat and bacteria in the follicle. This pattern is called acne mechanica.
Typical triggers include:
- tight athletic sets or compression tops
- backpacks, shoulder straps, or sports pads
- underwire bras or snug bands
- prolonged sitting (especially for buttock breakouts)
If your breakouts appear exactly where straps, seams, or gear sit, friction is usually part of the story.
Sweat, Heat, and Exercise
Sweat itself is not “dirty,” but sweat mixed with oil, dead skin, and friction can clog pores. The practical issue is timing: staying in damp clothing after workouts, re-wearing sports bras, or letting sweat dry repeatedly on the skin tends to sustain irritation.
Small changes make a difference:
- shower soon after exercise (gentle cleanse, not harsh scrubbing)
- change out of tight clothing promptly
- choose breathable fabrics for daily wear
- keep towels and gym gear clean and fully dried
Why Body Acne Can Be Harder to Treat Than Facial Acne
There are three reasons this tends to feel stubborn:
- Thicker skin and deeper folliclesInflammation can sit deeper, making lesions slower to flatten and more likely to leave marks.
- A larger surface areaCoverage is inconsistent. People treat “spots,” but the issue is often widespread follicle congestion.
- Daily triggers are harder to avoidClothing, heat, sweat, and pressure repeat every day. If those triggers aren’t addressed, even good products struggle.
Dinara often sees frustration here: patients do “everything right” for two weeks, then one cycle of sweating + friction brings it back. The solution is usually consistency and trigger control, not a new miracle product.
How to Treat Body Acne Effectively
At-Home Care
Home care is worth doing well, but it has to be realistic. Over-washing and aggressive scrubbing are common mistakes — they inflame the barrier and keep follicles reactive.
A solid home approach:
- cleanse once daily (or after sweating) with a gentle, acne-friendly wash
- use non-comedogenic body products (lotions, oils, sunscreens)
- avoid harsh scrubs, loofahs, and abrasive brushes
- don’t pick or “extract” body lesions (this drives marks and scars)
- keep clothing breathable and avoid repeated friction where possible
If breakouts are mild and mostly related to sweat or occasional occlusion, this can be enough. If they are persistent, painful, or leaving marks, home care alone often stalls.
Professional Body Acne Treatments
A structured body acne treatment plan in clinic tends to focus on two things: calming inflammation and improving how the follicle behaves long-term. The right mix depends on whether the acne is primarily inflammatory, comedonal (clogging-based), friction-driven, or hormone-driven.
Common professional options include:
- Medical-grade chemical peels for congestion, rough texture, and post-acne marks
- Laser and light-based treatments to reduce inflammation and help with lingering redness or early scarring
- Medical-grade skincare selected for tolerance on thicker body skin (often different than face products)
- A staged plan that accounts for workouts, uniforms, strap friction, and daily triggers
This is where results often shift: instead of chasing flare-ups, the plan reduces the conditions that cause them.
Body Acne Treatments at Philosophy of Beauty
At Philosophy of Beauty, the process starts with a skin assessment rather than a default product list. Dinara’s approach is conservative and practical: identify the dominant trigger (hormones, friction, sweat, product occlusion, or mixed factors), then build a plan that a patient can actually follow for months — because consistency is what changes recurrence.
Treatment plans may combine in-clinic technologies with targeted home care, with the goal of:
- reducing active inflammation
- preventing repeated follicle blockage
- improving skin texture and post-acne marks
- lowering the chance of scarring
If you’re noticing repeated flares in the same zones, or you’ve tried multiple routines without stable improvement, it’s usually time to consider professional acne treatment rather than cycling through stronger cleansers.
Clinical Quote
“Body breakouts are often treated like a hygiene problem. They’re not. They’re usually a trigger-and-inflammation problem. Once we identify the trigger pattern, the skin becomes much easier to calm.”
— Dinara, Founder & Registered Nurse, Philosophy of Beauty
FAQs
What causes body acne in adults?
Most adult cases involve a mix of hormones, friction, sweat, product occlusion, and ongoing inflammation.
Is body acne different from facial acne?
Yes. Body skin is thicker, follicles can be deeper, and products are harder to apply consistently.
Can exercise make body acne worse?
Exercise doesn’t cause acne, but sweat + friction + staying in damp clothing can worsen it.
How long does it take to see improvement with treatment?
Many people see early changes in 4–8 weeks, with more stable improvement over several months.
Are laser treatments effective for body acne?They can be, especially for inflammation, redness, and early scarring when used appropriately.
Can body acne leave scars?
Yes. Deeper inflamed lesions and repeated picking increase scarring risk.
When should I see a professional for body acne?
If breakouts are painful, persistent, widespread, recurring in the same zones, or leaving marks.
External References
- American Academy of Dermatology (AAD): acne overview and treatment principles
- Mayo Clinic: acne causes, risk factors, and treatment options
